On this page:
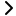 Breastfeeding your baby
Breastfeeding your baby
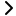 Continuing to breastfeed
Continuing to breastfeed
 Useful links
Useful links
Child and Family Health welcomes all families.
Child and Family Health Centres are staffed by registered nurses with recognised qualifications in the speciality of child and family health and offer:
- Breastfeeding advice and tips for all ages
- One on one support
Please contact your local centre for an appointment

 Breastfeeding your baby – Good things take time (NSW Health)
Breastfeeding your baby – Good things take time (NSW Health)
Breastfeeding is the normal and most valuable way to feed your baby. But breastfeeding is a skill that may take time, patience and practice both for mother and baby.
Breastmilk provides essential needs for growth, development and protection from illness. Babies receiving enough breastmilk don’t need water, juice or formula.
Your baby will use body language to let you know when they are hungry, these are called ‘feeding cues’. To learn more about ‘feeding cues’ you can watch videos on:
 Raising Children Network or
Raising Children Network or
 Australian Breastfeeding Association
Australian Breastfeeding Association
Your baby may want to feed 8-12 times in a 24-hour period, including overnight. This can mean feeding every 2-3 hours along with some cluster feeding, which is when your baby may feed several times in a couple of hours. As babies get older they tend to feed less often and the feeding time gets shorter.
But how do you know if your baby is getting enough milk? There should be at least 6 heavy wet nappies a day and the urine (wee) should be clear or very pale in colour and not smelly. If the urine is dark yellow and or has a strong smell, then you need to speak to a doctor. In the first few months your baby may have several bowel movements (poos) a day which may be very soft and runny. After that your baby may have not as many poos a day, but they may still be runny or soft.
Partners can support breastfeeding by:
- Changing nappies
- Bathing
- Settling
- Assisting with meals
- Caring for other children and pets
Partners can also learn about breastfeeding and offer their encouragement.
Child and Family Health Nurses will be able to help you with breastfeeding advice and support. A number of the Child and Family Health Nurses are also lactation consultants.

